All published articles of this journal are available on ScienceDirect.
Fetal Kidney Length in Gestational Age Prediction: A Comparative Study
Abstract
Background
Estimation of accurate gestational age is critical in perinatal care. Traditional fetal biometrics measured via ultrasonography face limitations, especially in the third trimester. Fetal Kidney Length (FKL) has emerged as a promising biometric parameter associated with advanced Gestational Age (GA). This study aimed to examine the diagnostic accuracy of FKL in comparison with traditional parameters in late pregnancy to optimize patient management and outcome.
Patients and Methods
A cross-sectional study enrolled 124 low-risk pregnant women with confirmed dating at 28-40 weeks of gestation. For every participant, two sets of data were collected: demographics (age, gravidity, date of last menstrual period) and fetal biometric parameters [Biparietal Diameter (BPD), Head Circumference(HC), Abdominal Circumference(AC), Femoral Length (FL), Amniotic Fluid Index(AFI), Estimated Fetal Weight (EFW), and Fetal Kidney Length (FKL)] including the length and width were calculated. Pearson's Correlation coefficients measured the strength of the association between GA and ultrasonic parameters.
Results
The mean KL for right and left (RKL, LKL) was 3.94±0.36 vs. 3.95±0.37 cm; p=0.84. FKL showed positive correlations with GA (r=0.54,0.52), p<0.001 for RKL, and LKL with determination coefficient r2= (0.29,0.27), respectively. GA was positively and strongly correlated to HC, AC, and FL with a correlation coefficient of 0.77, 0.76, and 0.73; p<0.001, respectively. The determination coefficient for the HC, AC, and FL were 0.29 and 0.27, respectively.
Conclusion
FKL showed a moderate link to GA during the third trimester; it did not surpass traditional fetal biometric parameters. Still, FKL measurement had advantages: consistent values, independence of feto-maternal condition, and non-invasiveness and acceptability. These qualities recommended FKL for integration into routine prenatal care as a supplementary metric when other parameter calculations are challenging. Further research is warranted to examine FKL performance when combined with other biometrics and explore its diagnostic and prognostic applications.
1. INTRODUCTION
Accurate estimation of fetal Gestational Age (GA) is a cornerstone in perinatal care. Precise estimation of GA can guide informed obstetric decisions, optimize intervention time, and facilitate patient risk stratification, thereby enabling the provision of tailored feto-maternal care [1, 2].
Currently, ultrasonic examination is one of the standard techniques for GA estimation through fetal biometric parameters. It offers a noninvasive, convenient, and widely acceptable tool for monitoring fetal development. The used fetal parameters: biparietal diameter, head circumference, abdominal circumference, and femoral length, are already established in daily practice; however, they are not without limitations [3].
They were subjected to potential inaccuracy owing to variabilities in fetal growth patterns, maternal risk factors, obesity, fetal lie and position, and population-specific differences [4-6].
For that, there was an increasing need for more fetal biometric parameters that could overcome these obstacles. Fetal Kidney Length (FKL) estimation has gained popularity in recent decades and was recommended as a potential parameter in GA estimation [7]. It was first discussed by Seoys et al. in 2003 as an additional parameter in the routine antenatal ultrasound scan [8].
Fetal kidney length demonstrates potential utility in practice due to its relative stability across various feto-maternal conditions, including fetal positioning, fetal growth restriction, and maternal obesity. FKL offered a more consistent estimate of GA, particularly for later stages of pregnancy, while the traditional methods face substantial limitations [7, 9].
Earlier works in the field had discussed encouraging the performance of FKL in GA estimation; however, some of these reports were inconsistent and showed contradicting results [10-13].
Moreover, the comparative utility of the standard fetal parameters remained largely unexplored.
The current study aimed to examine the performance of FKL in calculating GA among Iraqi pregnant women during 28–40 weeks of gestation compared to the fetal ultrasonic biometric, to examine their consistency with respect to the right and left kidneys, and to construct a nomogram value for FKL throughout the pregnancy. A comprehensive analysis of these parameters will determine whether FKL integration into the standard perinatal US exam can improve determining fetal gestational age, unveiling its potential use in practice.
2. PATIENTS AND METHODS
2.1. Study Design and Setting
A descriptive cross-sectional study was conducted in the radiological department at the maternity clinic of Al-Yarmouk Teaching Hospital from April 2023 through February 2024. The ethics committee of Mustansiriyah Medical College issued the study approval (IRB: 179; dated 23/12/2022). All procedures performed in the present study were in accordance with the ethical standards of the Helsinki Declaration and its amendments. Verbal consent was obtained from all patients before starting data collection and after explaining the aims of the study and assuring the confidentiality and anonymity of the participants. The study used convenience sampling to assess FKL performance in predicting Gestational Age (GA) for low-risk pregnant populations.
2.2. Inclusion Criteria
Uncomplicated singleton pregnancies in the third trimester, between 28 to 40 weeks of gestation, who are sure of the Last Menstrual Period (LMP) with regular menstrual cycle and without associated risk factors.
2.3. Exclusion Criteria
Pregnant with uncertain dates; chronic diseases and maternal complications, ex. chronic hypertension, diabetes mellitus, thyroid diseases, and gross maternal obesity (body mass index above 30 Kg /m2) were excluded. Other exclusion criteria are twin conception, fetal congenital anomalies, an abnormal amount of liquor (oligohydramnios, polyhydramnios), and fetal growth restriction. Each participant had two sets of data collected: demographics and ultrasonic parameters.
- Demographic criteria were collected through direct interviews with participants to cover personal history, including age, gravidity, date of last menstrual period, and past medical history. After a general and obstetrical examination, participants underwent a transabdominal ultrasound (US) examination.
- Ultrasound parameters: By the use of Samsung [Model No.S1ARM3HK4000057], equipped with a curved transducer of 3-5MHZ frequency, an assessment was made to fetal anatomy, fetal biometric parameters: [Biparietal Diameter (BPD), Head Circumference(HC), Abdominal Circumference(AC), Femoral Length (FL), Amniotic Fluid Index(AFI), Estimated Fetal Weight(EFW) via Hadlock's method] and Fetal Kidney Length (FKL).
2.4. Fetal Kidney Length Measurement
Fetal kidneys were visualized in both transverse and longitudinal planes. The right (RT) was marked using the liver as a landmark. At the same time, the left (LT) kidney was marked in the stomach as a reference.
To calculate the FKL, the probe was oriented at a right angle on either side of the abdominal aorta to get the largest longitudinal length of the two kidneys.
After identifying the upper and lower poles of the kidneys, the FKL was estimated from the outer edge of the upper pole to the outer edge of the lower pole in the sagittal plane, along the longitudinal axis, using electronic calipers (Fig. 1). Each measurement was repeated two times, and the mean value was recorded. A single experienced sonographer (with an interest in fetal medicine and 22 years of experience) made all measurements to ensure data robustness. These steps were endorsed to reduce intra-observer errors and inter-observer errors. In the end, the study included 124 participants who were eligible for the inclusion criteria.
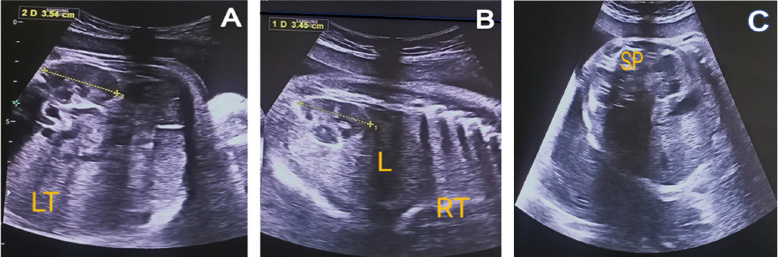
At 31 weeks, an abdominal ultrasonography was taken to assess the fetal abdomen at the level of the kidneys. (A and B) present sagittal views, demonstrating kidney length measurement =3.54cm and the right kidney = 3.45cm. L: Liver; RT: Right; LT: Left; SP: spine. (C) depicts a transverse view.
2.5. Sample Size Calculation
For cross-sectional studies, the sample size required can be estimated according to the following formulae: N = (Zα/2 + Zβ2) / r2 [14].
Z-score equivalent to a two-tailed significance level (for α = 0.05, Zα/2 ≈ 1.96). Zβ: Z-score equivalent to the power decided by the researcher (for power = 0.8, Zβ ≈ 0.84). As for r, it stands for correlation taken from earlier studies, 0.27 [13].
(Zα/2 + Zβ)2 = (1.96 + 0.84)2 = 7.84 . The r2 = (0.27)2 = 0.0676.
N = (7.84) / (0.0676) = 117.11≈ 118 participants
2.6. Statistics
The collected data were entered into Microsoft Excel 2016 and analyzed using the SPSS version 26 statistical program. An independent two-sample t-test was employed to assess the difference between the mean lengths of the right and left kidneys. Correlation coefficients between each measured predictor variable and gestational age were calculated using Pearson’s correlation test, along with linear correlation analysis. Logistic regression was constructed to estimate the 95% Confidence Intervals (CI) and corresponding p-values for the key measurement in the study, including FKL and correlation coefficients, which adds precision to calculation and insight into data variability. A post-hoc test was employed to confirm the study's strength. A p-value of 0.05 was considered as the threshold for statistical significance.
3. RESULT
The majority of the study participants, 79 (64%) were aged between 20- 30 years, while 34(27%) were >30 years, and 11 (9%) were < 20 years. Most of the cases were multiparous: 81(65%) compared to 43 (35%) primigravidae. The ultrasonic criteria of the participants are summarized in Table 1. The mean gestational age based on LMP was 34.57±2.3 weeks, and the mean diameters for the RK and LK were 3.94±0.36 3.95±0.37 cm, respectively. The kidneys' mean lengths are compared in Table 2, revealing no significant differences; p=0.84.
The distribution of both kidneys' lengths based on the weeks of gestation (28-40 weeks) is shown in Table 3. This shows a steady increase alongside weeks of gestation, up to 38 weeks. The strength of the association between GA versus ultrasonic fetal parameters was tested by Pearson analysis in Table 4. with the regression equation used. The GA was strongly and positively correlated to HC, AC, and FL with a correlation coefficient of (0.77,0.76,0.73); p<0.001, respectively. The determination coefficient showed values of 90.59, 0.58, and 0.53, respectively. The RKL and LKL were moderately and positively linked to GA with r=0.54, 0.52; p<0.001, respectively. Likewise, the determination coefficient scored 0.29 and 0.27, respectively, with confidence intervals 0.42-0.61 and 0.45-0.63, and regression equation; GA=17.46+4.35*RKL and GA=18.3+ 4.12*LKL for the RT and LT, respectively.
| Study Parameters (n=124) | Minimum | Maximum | Mean± Std. Deviation |
|---|---|---|---|
| Gestational age according to LMP (weeks) | 28 | 40 | 34.57±2.3 |
| Right Kidney length (cm) | 3.00 | 4.90 | 3.94±0.36 |
| Left Kidney length (cm) | 3.00 | 4.95 | 3.95±0.37 |
| Biparietal diameters (cm) | 6.91 | 9.72 | 8.63±.65 |
| Head circumference (cm) | 25.42 | 34.38 | 31.14±1.93 |
| Abdominal circumference (cm) | 21 | 35.85 | 30.48±3.29 |
| Femoral length (cm) | 4.96 | 7.99 | 6.77±0.63 |
| Estimated fetal weight (Gram) | 1055 | 3500 | 2198±287 |
| KL | N | Mean(cm) | Std. Deviation | p-value |
|---|---|---|---|---|
| RKL | 124 | 3.94 | 0.36 | 0.708 |
| LKL | 124 | 3.95 | 0.37 |
| GA (weeks) | Number of Cases | Right Kidney Mean±Std. Deviation (cm) |
Left Kidney Mean ±Std. Deviation (cm) |
|---|---|---|---|
| 28 | 3 | 3.30 ±0.30 | 3.40±0.26 |
| 29 | 6 | 3.43 ±0.34 | 3.62±0.10 |
| 30 | 7 | 3.64±0.19 | 3.60±0.20 |
| 31 | 6 | 3.60±0.09 | 3.66±0.12 |
| 32 | 4 | 3.70±0.39 | 3.68±0.46 |
| 33 | 12 | 3.73±0.28 | 3.92±0.29 |
| 34 | 15 | 4.02±0.30 | 3.94±0.28 |
| 35 | 18 | 4.07±0.28 | 4.16±0.38 |
| 36 | 26 | 4.06±0.38 | 4.06±0.36 |
| 37 | 8 | 4.13±0.23 | 4.04±0.11 |
| 38 | 6 | 4.08±0.25 | 4.02±0.35 |
| 39 | 11 | 3.95±0.29 | 4.20±0.54 |
| 40 | 2 | 4.08±0.17 | 4.07±0.04 |
| Parameters | Correlation Coefficient (r) | 95% Confidence Interval (CI) | p-value | Regression Equation | Determination Coefficient (r2) |
Effect Size |
|---|---|---|---|---|---|---|
| Correlation of GA versus RKL | 0.54 | [0.45-0.63] | <0.001 | GA=17.46+4.35*RKL | 0.29 | Medium |
| Correlation of GA versus LKL | 0.52 | [0.42-0.61] | <0.001 | GA=18.3+4.12*LKL | 0.27 | Medium |
| Correlation of GA versus BPD | 0.69 | [0.61-0.76] | <0.001 | GA=8.12+3.06*BPD | 0.47 | Large |
| Correlation of GA versus HC | 0.77 | [0.70-0.82] | <0.001 | GA=1.58+1.16*HC | 0.59 | Large |
| Correlation of GA versus AC | 0.76 | [0.69-0.81] | <0.001 | GA=13.97+0.68*AC | 0.58 | Large |
| Correlation of GA versus FL | 0.73 | [0.66- 0.79] | <0.001 | GA=11.61+3.39*FL | 0.53 | Large |
4. DISCUSSION
Our analysis demonstrated that the mean fetal KL linearly increased with GA up to the 38th week. FKL was comparable between the RK and LK during the third trimester. Moreover, they were positively and significantly correlated to GA. However, the determination coefficient of the KL did not exceed that of other standard fetal biometry markers (HC, AC, FL).
Estimating the exact GA is of paramount importance in tracking fetal and maternal wellbeing [2, 15].
However, it can be quite challenging, especially during the third trimester when the traditional US biomarkers cannot be dependable. An evaluation was made of the utility of FKL in GA determination, aiming to provide an additional metric for calculating GA when other parameters are difficult to obtain and will optimize the patient's management and outcome [16].
Earlier studies align with our results, confirming a positive correlation between KL and advanced GA; it appears that KL increased by 1 cm each month [10, 17-19]. The analysis also confirmed no significant difference between the measurements of the RT and LT kidneys, which is consistent with most published studies [9, 10, 17, 20].Kiridi et al. examined the length, width, and anteroposterior diameter of the fetal kidneys in Nigerian women from 20-40 weeks of gestation. In accordance with our result, a positive correlation was proved with r=0.89,0.87,0.83, respectively, and r2=0.79, which is higher than our results. Moreover, they discussed that maternal height was positively and significantly linked with fetal kidney measurement, while maternal weight had no impact [21].
Eissa et al. examined FKL measurement among Egyptian pregnant ladies at GA from 20-40 weeks. They confirmed a positive link between FKL and GA, and they found no significant differences between the RK and LK that were in line with our results. Their analysis shows a strong positive correlation between FKL and other ultrasonic parameters, recommending FKL as an accurate predictor for GA estimation with (r2 = 0.95) [22].
Kaul et al. tested FKL performance among the Indian population between 24-41 weeks of gestation. They showed significant LKL measurement across all gestational ages. A positive link was proven with other fetal biometric parameters. They recommended FKL as the most reliable parameter for A estimation, surpassing FL and BPD. Surprisingly, AC was the least reliable in GA estimation. Similarly, an earlier study by Konje among English pregnant women at 24 to 38 weeks reported comparable findings, recommending the use of combined biometric models to reduce the standard error in GA estimation from approximately eight days to within 2 days [11, 12].
The discrepancy between the last study's results and those reported by others may be attributed to more than one reason. Both Kaul et al. and Konje et al. studies were limited by small sampling power [23]. They did not address confounders like sociodemographic or inter-observer variability. Additionally, the use of old ultrasonic devices in their studies (since both took place in 2012 and 2002, respectively) is likely to contribute to measurement inaccuracy [11, 12, 23].
Choudhary et al. evaluated the value of FKL as a marker of fetal biometry among Indian pregnant women at 22-40 weeks of gestation. Their results confirmed a strong positive correlation between the two, with agreement strength exceeding 0.99%. Their results recommended FKL as a supplementary standard fetal parameter during late pregnancy [7], which is in line with our results.
An earlier Iraqi study conducted in Tikrit province demonstrated a linear increase in Kidney Length (KL) measurements from 20 to 38 weeks of gestation, showing a positive correlation between fetal kidney length and GA (r=0.34). The strength of the association with GA was weaker for FKL compared to AC and HC, with correlation coefficients of r = 0.75 and r = 0.71, respectively. Their study discussed meaningful differences between the RK and LK lengths, p < 0.001, in contrast with most published works. The unique racial diversity in Tikrit province may explain the observed differences in kidney lengths added to a small sampling bias [13].
The determination coefficient [r2] in the current study revealed that HC, AC, and FL estimation for GA surpassed FKL with r2=0.59,0.58,0.53 vs. r2= 0.29 and 0.27 for the RK and LK, respectively.
The current analysis confirmed the limitation of FKL as a predictor of GA. When comparing the standard biometric US parameters, the FKL had lower predictive power. Several factors may lead to this moderate correlation.
The sample under study was low risk; a more diverse sample may perform better. It is important to note that, unlike other organs, KL may be less affected by growth retardation, making the FKL measurement less sensitive to growth changes among normal pregnant individuals. Another point is the inherent difficulty in defining KL parameters as a soft organ compared to significant solid organs such as the head and femur, not to mention the active fetal movement during the third trimester.
We had to acknowledge study limitations, including potential selection bias since only a low-risk population was included and data was collected from a single center; both impose challenges in the globalization of the results.
The FKL as a parameter shows wide diversity across geographical regions and exhibits racial differences, as observed in Tikrit [20]. Another limiting point is the cross-sectional design of this study, which hinders its ability to establish actual causation [21].
Future studies should address these limitations to improve our understanding of FKL application in obstetrics. Another promising area in GA determination is the role of Artificial Intelligence (AI) technology, which may evolve FKL from a supplementary tool to a central tool in GA measurement, especially during the third trimester. Applications of Machine learning can identify subtle growth changes that traditional biometric parameters might overlook and help generate population-specific prediction equations for GA determinations [24–26].
Calculating FKL is technically easy and may serve as a valuable auxiliary metric for the determination of GA, mainly when fetal positioning makes other measurements, such as FL, challenging [27]. Besides, FKL displays consistent stability throughout the third trimester in contrast to BPD, which may be less reliable in late pregnancy, or the AC, whose measurement becomes a challenge in cases with low amnion or low fetal weight [28]. Although FKL shows lower predictive power, it may serve as a valuable adjunct to traditional fetal parameters.
| Study Type, No., Parameters Tested |
Main Finding | References |
|---|---|---|
| • Prospective • Turkey • 180 pregnant • Standard fetal biometry added to amniotic fluid index(AFI) &FKL |
• Positive correlation between GA & FKL fetal kidney length (r=0.9). • FKL negatively correlated with AFI. • The study incorporated FKL in GA estimation, leading to a higher determination coefficient from 0.965 up to 0.987. |
Ugur et al. 2016 [17] |
| • Prospective • India • 120 pregnant at 20-40weeks • Standard fetal biometry added to FKL |
• The study added a regression formula to GA prediction, which yielded an improved fit for GA prediction, with a determination coefficient of 0.97 when compared to traditional biometrics. • Femur length, when added, leads to better performance. |
Bharatnur et al. 2021 [32] |
| • Prospective • Nepal • 250 pregnant at 24-<40 weeks • Standard fetal biometry added to FKL |
• The FKL was positively correlated to GA with r=0.9 • They confirmed a more efficient GA prediction when FKL was added to measured parameters on ultrasound. • Determination coefficient improved from 0.918 to 0.936 |
Gautam et al. 2022 [33] |
What is novel about this study is that it sets the norms for FKL measurement among the Iraqi population. Previous work was limited by small sample sizes, which led to a discrepancy in the reported FKL of both kidneys (RT and LT), adding to a weak correlation coefficient. By addressing these restrictions, we can have reliable, consistent data for FKL to improve accuracy in GA determination.
This study has several strengths, including a robust sample size, a study setting at a tertiary institution, and the involvement of a skilled radiologist, which minimized inter-observer variability [29]. To reduce potential bias, we limit the collected sample to a low-risk population of the same racial background [30, 31].
We believe that the current results have clinical application in practice. One of them is the improved accuracy of GA determinations by integration of FKL to routine ultrasound examination, which was discussed by other researchers and summarized in Table 5 [17, 31-33].
Another significant point is the FKL applicability throughout different trimesters. This versatility is a notable strength that addresses limitations associated with traditional fetal biometrics, particularly during the third trimester [34, 35]. Abony et al. have emphasized the importance of establishing reference values for FKL specific to each population to enhance measurement accuracy [36].
We recommend longer studies that enroll high-risk populations across diverse racial groups to assess FKL reliability among different populations [37]. Additionally, the integration of FKL with other ultrasonic parameters or even better AI-based technology may enhance FKL predictive accuracy and broaden its applicability in obstetrical care [38, 39].
CONCLUSION
FKL is a valuable supplement tool for gestational age determination during the third trimester. It is accessible, acceptable, consistent, and has a strong relationship with advanced GA, which makes it an effective tool for obstetricians, especially when traditional fetal biometrics are difficult to examine. Incorporating FKL into routine perinatal ultrasound exams can improve precision and improve maternal outcomes. Future research is warranted to explore applications of advanced biometric parameters and AI technology to maximize its diagnostic and prognostic avenues.
AUTHORS’ CONTRIBUTION
All authors contributed equally to the manuscript's conception, literature search, writing, editing, and revising. All authors read and agreed on the final version.
LIST OF ABBREVIATIONS
| FKL | = Fetal Kidney Length |
| GA | = Gestational Age |
| BPD | = Biparietal Diameter |
| HC | = Head Circumference |
| AC | = Abdominal Circumference |
| FL | = Femoral Length |
| AFI | = Amniotic Fluid Index |
| EFW | = Estimated Fetal Weight |
ETHICS APPROVAL AND CONSENT TO PARTICIPATE FOR PUBLICATION
The ethics committee of Mustansiriyah Medical College, Iraq issued the study approval (IRB: 179; dated 23/12/2022).
HUMAN AND ANIMAL RIGHTS
All human research procedures followed were in accordance with the ethical standards of the committee responsible for human experimentation (institutional and national), and with the Helsinki Declaration of 1975, as revised in 2013.
AVAILABILITY OF DATA AND MATERIALS
The data supporting this work is available from the corresponding author [W.S] at a reasonable request.
ACKNOWLEDGEMENTS
The authors would like to thank Mustansiriyah University for its continuous support.


